Healthcare
Healthcare in Nigeria

At a population of around 190 million, Nigeria is the most populous country in Africa, and the largest economy on the continent. While various health indicators in Nigeria have shown steady improvement, progress has nonetheless been slow, and the country faces numerous healthcare delivery challenges. Socioeconomic disparities across geopolitical zones, states and rural and urban areas increase health insecurity, and pervasive poverty, high levels of (especially youth) unemployment, and poor access to clean water and sanitation in many areas increases the risk of communicable disease, malnutrition, and childhood and maternal mortality. Uneven development between states and regions – exacerbated by conflict, drought, and public health crises or epidemics – and a lack of medical infrastructure, equipment and personnel in many areas has resulted in poor public healthcare delivery for the majority of the population. The following country statistics, from the World Health Organization 2018 statistics report, provide an indication of the health challenges facing the country:
- Life expectancy at birth: 55.7
- Maternal mortality: 814 deaths per 100 000 live births
- Under-5 mortality: 104.3 per 1000 live births
- Malaria incidence: 349.6 per 1000 population
- Tuberculosis incidence: 219 per 1000 population
- Stunting among children under five: 43.6%
- Density of physicians: 0.4 per 1000 population
- Density of nurses and midwives: 1.5 per 1000 population
- Domestic general government health expenditure (GGHE-D) as a percentage of general government expenditure (GGE): 5.3%
Development Africa is committed to working with public and private partners to strengthen healthcare delivery throughout Nigeria. Healthcare programmes include the establishment and management of health facilities, medical infrastructure development and refurbishment, community healthcare interventions, training and capacity development, and malaria elimination initiatives, among others.
FAMILY CARE IKOTA MEDICAL CENTRE

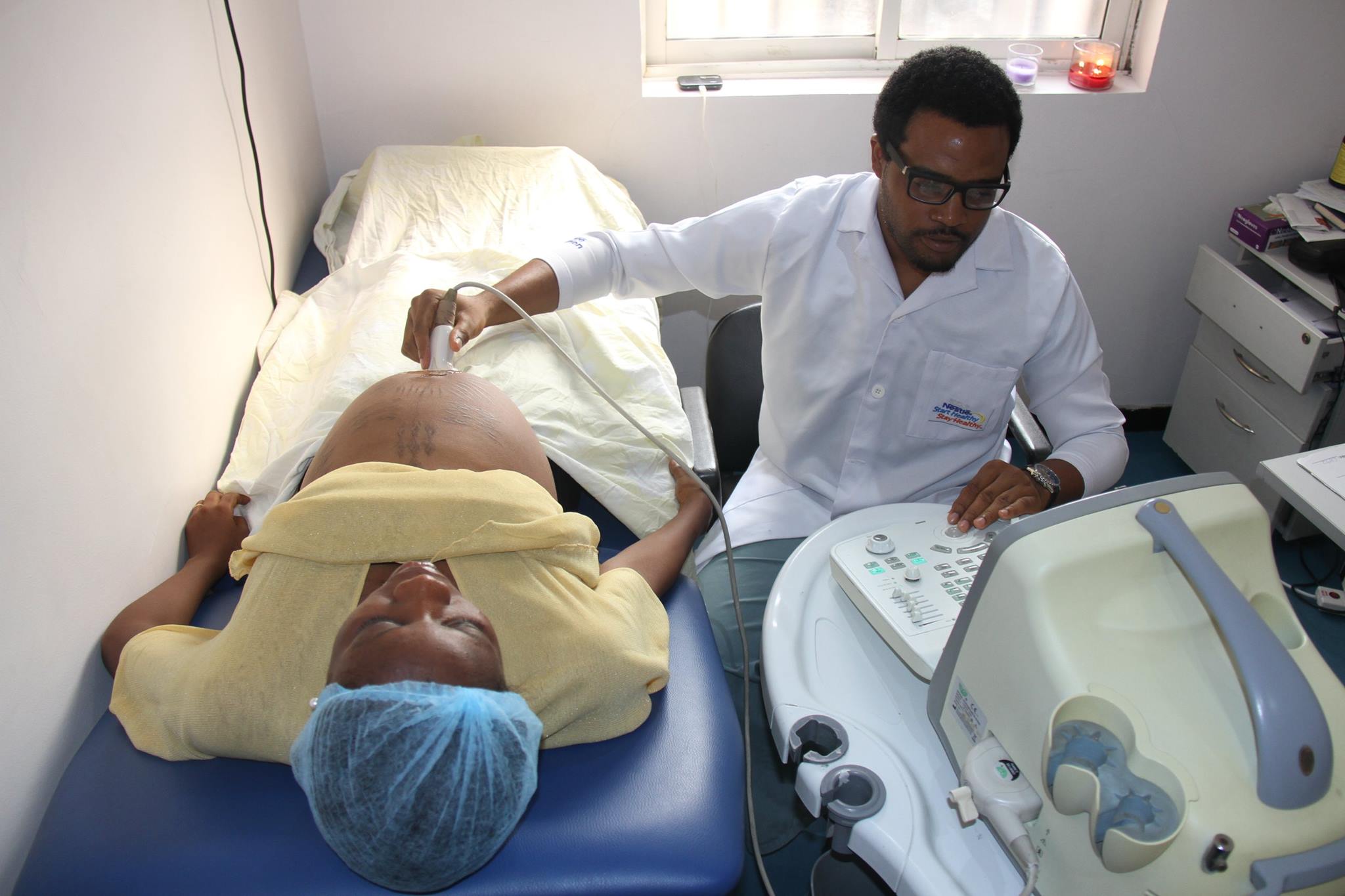
The Family Care Ikota Medical Centre (FCIMC) is a Development Africa model healthcare facility. The centre provides 24-hour medical care and attention to low-income families across Lagos State. The centre is equipped with patient wards, a maternity delivery room, an operating theatre, consultation rooms, a pharmacy, a laboratory, and modern medical equipment and ultrasound services. The FCIMC has contributed to reducing malaria prevalence and infant mortality rates, improving maternal healthcare, and lowering the number of medical emergencies in the community.
The cost to patients at the FCIMC is considerably lower than at surrounding commercial clinics, and sponsorship is available for those who cannot afford the subsidised price. The centre provides a skilled and professional environment in which to treat both routine and life-threatening cases, while promoting health education on various topics including vaccinations, hygiene, maternity and infant care, malaria, and HIV/AIDS awareness.
In line with Development Africa’s commitment to sustainability and renewable resource initiatives, the FCIMC is also equipped with a solar-powered backup system, solar-powered water heaters, and energy-efficient lights and medical equipment.
MEDICAL INFRASTRUCTURE DEVELOPMENT
In order to address specific gaps in the public healthcare system, Development Africa’s Medical Infrastructure Development programme designs and builds sustainable and specialised medical facilities in various locations. This involves extensive research and planning, as well as engagement with the communities themselves to identify key needs and requirements.
In recent years, Development Africa has established a number of Maternity Referral Centres across Nigeria, which are fully equipped for the safe delivery of children in each community. The model design includes a delivery room /theatre, a twelve-bed ward for recovering mothers, a nurses’ station, an ultrasound room, and a hall for antenatal training.
COMMUNITY HEALTHCARE INTERVENTION
Development Africa’s Community Healthcare Intervention programme brings free, quality healthcare services directly to communities. With the participation of a large team of medical professionals, the programme organises free medical treatment for community members over the project duration at a target location.
Specialists from various fields—including general practitioners, paediatricians, surgeons, gynaecologists, anaesthesiologists, ophthalmologists, optometrists, and dentists—work intensively to deliver a wide range of services to community members over the duration of the project. To date, 94 interventions in 21 different states have provided medical assistance to 293,699 people.
Alongside providing free medical treatment throughout each project, the Community Healthcare Intervention programme also emphasises the need for sustainable healthcare strategies. Development Africa provides training for the local medical staff and personnel, so as to facilitate the provision of reliable medical care after or between projects.
During the Community Healthcare Intervention, members of the target locations receive:
- Consultation and medication
- Dental procedures
- General surgical procedures and operations
- Ophthalmic procedures (including ophthalmic surgeries)
- Optometric examinations and prescription eyeglasses
- Capacity development for community medical personnel
HEALTHCARE CAPACITY DEVELOPMENT
In partnership with healthcare professionals and agencies, Development Africa has established a series of practical training lectures to improve the delivery of healthcare services across Nigeria.
Case Management of Malaria at the Primary Health Care Centre
Healthcare workers play a vital role in the diagnosis, treatment, and prevention/control of malaria. It is therefore important that they are fully aware of and understand current diagnostic procedures and appropriate treatment, national policies, prevention methods, and recommended courses of action. The training manual used is a unified training guide/module for all Roll Back Malaria (RBM) partners in Nigeria, and was created by the Federal Ministry of Health/National Malaria Elimination Programme, in conjunction with Development Africa and other RBM partners. The training covers many aspects essential to understanding, identifying, and treating malaria, such as aetiology, transmission, pattern of presentation, and methods of diagnosis.
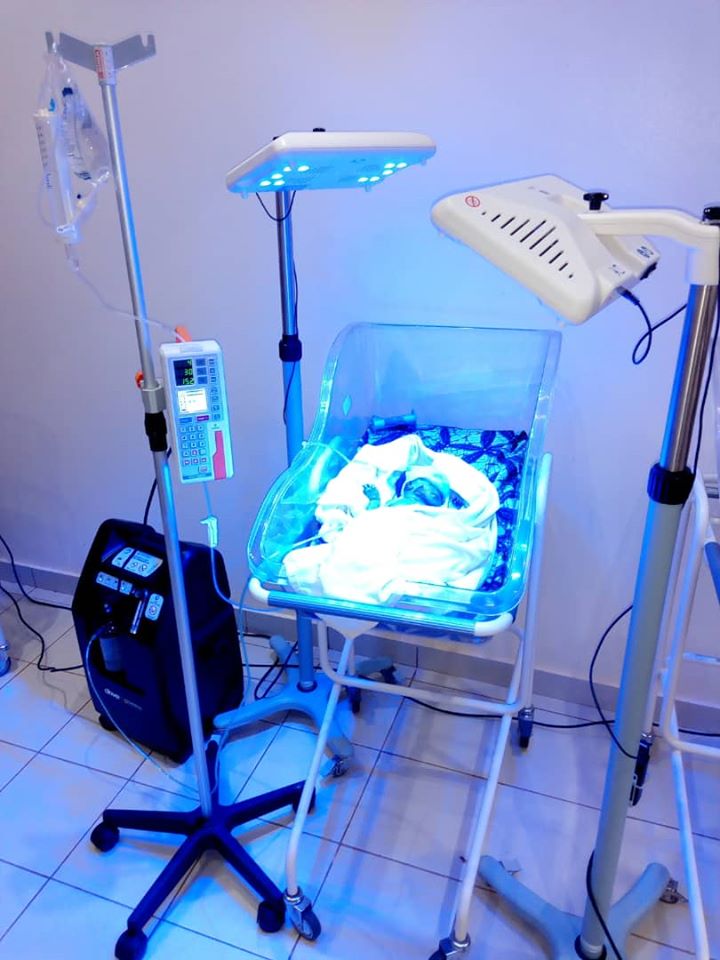
Hospital-Acquired Infections
Hospital-born babies are at increased risk of neonatal infections in developing countries, because of poor intrapartum and postnatal infection control practices. This interactive training addresses those issues and discusses the best ways in which they can be avoided.
Management of Obstetric Haemorrhage
Obstetric haemorrhage is a leading cause of maternal mortality, with postpartum haemorrhage (PPH) accounting for the majority of these deaths. Obstetric haemorrhage is often sudden and unexpected, and early recognition and treatment is essential to ensure a positive outcome. The training covers current practice and recommended courses of action to effectively identify and treat obstetric haemorrhage.
Malaria Elimination Programme
In 2009, in collaboration with the Federal Ministry of Health/National Malaria Elimination Programme, Development Africa created a malaria control initiative. Branded as the Development Africa Malaria Elimination Programme (DAMEP), its goal is to reduce the malaria burden in target states through recommended interventions. These include distribution of LLINs, high-impact awareness campaigns, capacity building for healthcare workers and students, Intermittent Preventative Treatment for pregnant women, etc. DA works in collaboration with the State and Federal Ministries of Health.